COPD (Chronic Obstructive Pulmonary Disease)
Introduction
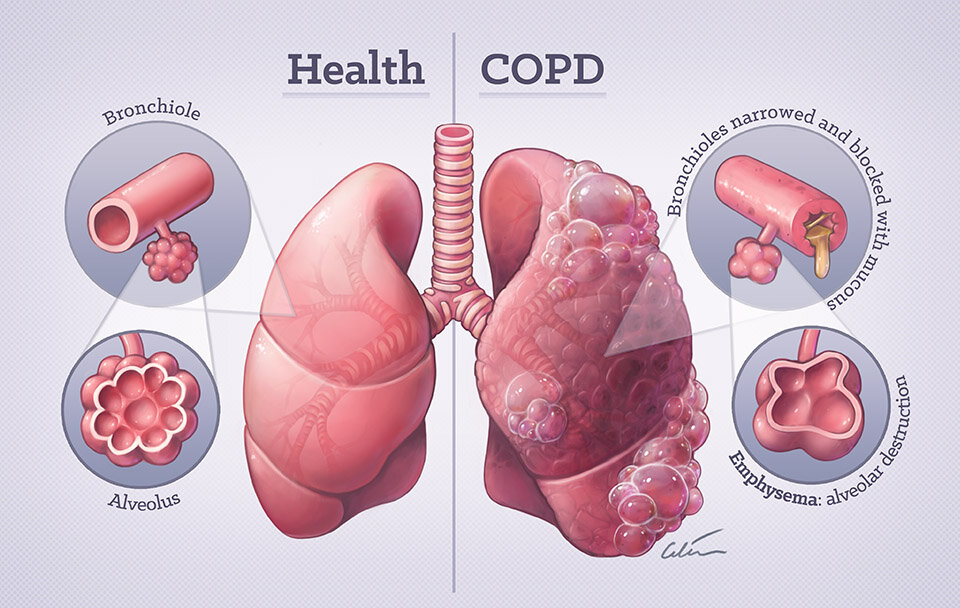
Chronic Obstructive Pulmonary Disease (COPD) is a progressive and debilitating respiratory condition that affects the lungs and the body’s ability to breathe effectively. It is a chronic inflammatory disease that causes obstructed airflow from the lungs, making it increasingly difficult to breathe over time. COPD is a umbrella term that includes two main conditions: chronic bronchitis and emphysema.
Causes
Chronic Obstructive Pulmonary Disease is primarily caused by exposure to harmful particles or gases that irritate and damage the lungs. The most common cause of COPD is:
- Tobacco smoke: Cigarette smoking is the leading cause of COPD, accounting for approximately 90% of cases. Both firsthand and secondhand smoke exposure can contribute to the development of COPD.
- Environmental exposures: Long-term exposure to air pollutants, chemical fumes, and occupational dusts (such as coal dust, silica dust, or asbestos) can increase the risk of developing COPD, particularly in individuals with a genetic predisposition.
- Alpha-1 antitrypsin deficiency: This is a rare genetic disorder that can cause COPD due to a lack of a protein called alpha-1 antitrypsin, which is essential for protecting the lungs from damage.
Risk Factors
- Smoking: Both current and former smokers are at a higher risk of developing COPD. The risk increases with the duration and intensity of smoking.
- Age: The risk of Chronic Obstructive Pulmonary Disease increases with age, as lung function naturally declines over time.
- Occupational exposure: Individuals who work in environments with high levels of dust, chemicals, or fumes have an increased risk of developing COPD.
- Genetics: Having a family history of COPD or a genetic predisposition, such as alpha-1 antitrypsin deficiency, can increase the risk.
- Respiratory infections: Frequent respiratory infections, especially in childhood, can damage the lungs and contribute to the development of COPD later in life.
- Exposure to secondhand smoke: Exposure to secondhand smoke, particularly during childhood or in the home, can increase the risk of Chronic Obstructive Pulmonary Disease.
Symptoms
- Persistent cough: A chronic cough that may produce mucus or phlegm is a common symptom of COPD.
- Shortness of breath: Individuals with COPD often experience breathlessness, especially during physical activity or exertion.
- Wheezing: A whistling or wheezing sound when breathing is common in COPD patients.
- Chest tightness: A feeling of tightness or constriction in the chest area may occur due to airway obstruction.
- Fatigue: The increased effort required to breathe can lead to fatigue and weakness.
- Frequent respiratory infections: It can make individuals more susceptible to respiratory infections, such as bronchitis or pneumonia.
Complications
If left untreated or poorly managed, COPD can lead to various complications, including:
- Respiratory failure: In advanced stages of COPD, the lungs may struggle to provide enough oxygen to the body, leading to respiratory failure.
- Heart problems: The strain on the lungs and reduced oxygen levels can put additional stress on the heart, increasing the risk of heart disease, arrhythmias, and heart failure.
- Exacerbations: Chronic Obstructive Pulmonary Disease exacerbations, or flare-ups, are periods when symptoms become significantly worse, often due to respiratory infections or exposure to environmental triggers.
- Lung cancer: Individuals with COPD have an increased risk of developing lung cancer, particularly if they are or were smokers.
- Depression and anxiety: The physical limitations and challenges associated with COPD can contribute to mental health issues, such as depression and anxiety.
Differential Diagnosis
COPD shares some symptoms with other respiratory conditions, and it is important to differentiate it from these conditions for proper diagnosis and treatment. The differential diagnosis for Chronic Obstructive Pulmonary Disease may include:
- Asthma: While both asthma and COPD involve airway obstruction and breathing difficulties, asthma is typically reversible and episodic, while COPD is progressive and irreversible.
- Bronchiectasis: This condition is characterized by abnormal dilation and scarring of the bronchial tubes, leading to persistent cough, mucus production, and recurrent respiratory infections.
- Lung cancer: Lung cancer can cause symptoms similar to COPD, such as persistent cough, shortness of breath, and wheezing.
- Pulmonary fibrosis: This condition involves the scarring and stiffening of lung tissue, making it difficult to breathe and potentially leading to respiratory failure.
- Heart failure: Symptoms like shortness of breath and fatigue can be caused by heart failure, which may be misdiagnosed as Chronic Obstructive Pulmonary Disease.
Preventions
- Smoking cessation: Quitting smoking is the most effective way to prevent or slow the progression of COPD. Smoking cessation programs and medications can provide support and increase the chances of success.
- Avoiding exposure to pollutants: Minimizing exposure to air pollutants, dust, and chemical fumes in the workplace and at home can reduce the risk of developing COPD.
- Vaccination: Regular vaccination against influenza and pneumonia can help prevent respiratory infections that may exacerbate COPD symptoms.
- Early diagnosis and treatment: Early detection and appropriate treatment of COPD can help manage symptoms and slow the progression of the disease.
- Maintaining a healthy lifestyle: Regular exercise, a balanced diet, and maintaining a healthy weight can improve overall respiratory health and reduce the risk of Chronic Obstructive Pulmonary Disease complications.
Diagnosis
- Medical history and physical examination: The healthcare provider will take a detailed medical history, including smoking history and exposure to environmental pollutants, and perform a physical examination to assess respiratory function.
- Pulmonary function tests: Spirometry is the primary diagnostic test for COPD, measuring lung function by assessing airflow and lung volumes. Other tests, such as diffusing capacity tests, may also be performed.
- Chest imaging: Chest X-rays or CT scans can help identify structural changes in the lungs and rule out other conditions.
- Blood tests: Blood tests may be ordered to check for other underlying conditions or to assess the levels of oxygen and carbon dioxide in the blood.
- Alpha-1 antitrypsin deficiency testing: In some cases, genetic testing for alpha-1 antitrypsin deficiency may be recommended, especially in individuals with a family history or early onset of COPD.
Treatments
COPD is a chronic and progressive condition that requires ongoing management and treatment. The goals of treatment are to alleviate symptoms, improve quality of life, and slow the progression of the disease. Treatment strategies may include:
- Bronchodilators: These medications, such as albuterol or tiotropium, help relax and open the airways, making it easier to breathe.
- Inhaled corticosteroids: These anti-inflammatory medications, often used in combination with bronchodilators, can help reduce airway inflammation and prevent exacerbations.
- Oxygen therapy: Supplemental oxygen may be prescribed for individuals with severe COPD and low blood oxygen levels to improve oxygenation and reduce the strain on the heart and lungs.
- Pulmonary rehabilitation: This comprehensive program combines exercise training, education, and nutritional counseling to improve overall physical and mental health for individuals with COPD.
- Medications for exacerbations: During COPD exacerbations, additional medications, such as oral corticosteroids or antibiotics, may be prescribed to manage symptoms and treat underlying infections.
- Surgery: In some cases, surgical interventions like lung volume reduction surgery or lung transplantation may be considered for individuals with severe COPD and specific eligibility criteria.
- Lifestyle modifications: Quitting smoking, engaging in regular physical activity, maintaining a healthy diet, and avoiding exposure to environmental pollutants are essential lifestyle changes for individuals with COPD.
Important Key Points
- COPD is a progressive respiratory condition that causes obstructed airflow and breathing difficulties.
- It includes two main conditions: chronic bronchitis and emphysema.
- The primary cause is exposure to tobacco smoke, with environmental pollutants and a genetic disorder (alpha-1 antitrypsin deficiency) also contributing.
- Risk factors include smoking, age, occupational exposures, genetics, respiratory infections, and secondhand smoke exposure.
- Symptoms include persistent cough, shortness of breath, wheezing, chest tightness, fatigue, and frequent respiratory infections.
- Complications can arise, such as respiratory failure, heart problems, exacerbations, lung cancer, depression, and anxiety.
- Differential diagnosis includes asthma, bronchiectasis, lung cancer, pulmonary fibrosis, and heart failure.
- Prevention involves smoking cessation, avoiding pollutants, vaccination, early diagnosis, and maintaining a healthy lifestyle.
- Diagnosis utilizes medical history, physical examination, pulmonary function tests (spirometry), chest imaging, blood tests, and genetic testing.
- Treatment aims to alleviate symptoms, improve quality of life, and slow progression through bronchodilators, inhaled corticosteroids, oxygen therapy, pulmonary rehabilitation, medications for exacerbations, and surgery in severe cases.
- Lifestyle modifications, such as quitting smoking, exercise, diet, and avoiding pollutants, are crucial.
- A multidisciplinary approach with healthcare professionals is essential for effective COPD management.
Note: This is a general overview, and it’s always best to consult with a healthcare professional for personalized medical advice and treatment.
